Treatment
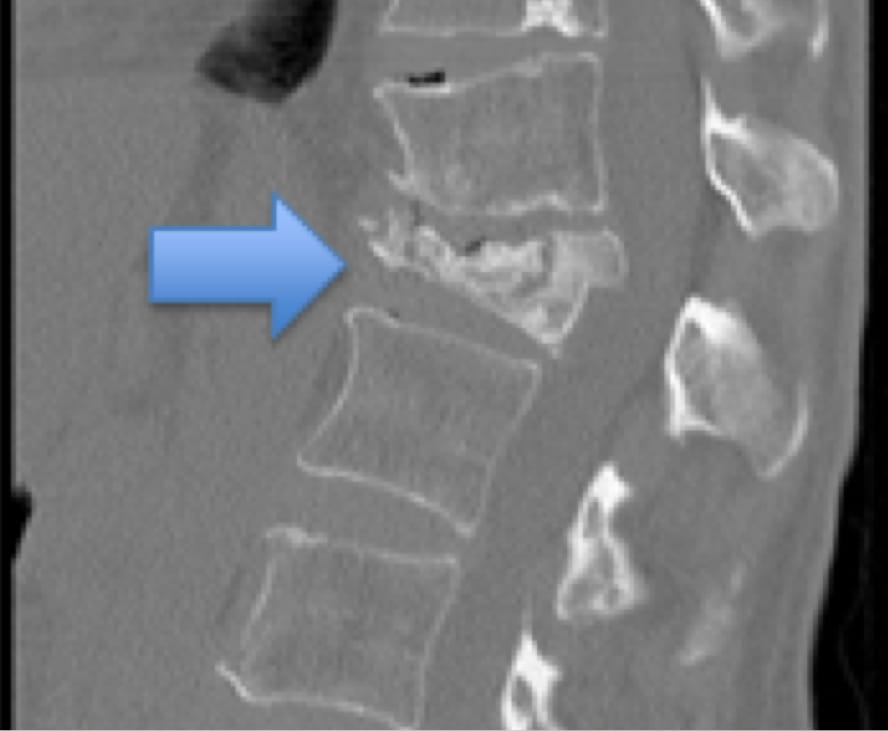
Just one fracture can disrupt the alignment of the spinal column and put stress on adjacent vertebrae, thereby increasing the risk for another fracture. Left untreated, the broken vertebra will eventually heal in its fractured position. Dr. Stieber’s approach involves medical management of the underlying disorder (e.g., osteoporosis) in addition to repair of the broken bone.
Two minimally-invasive procedures that can alleviate the pain of compression fractures are vertebroplasty and balloon kyphoplasty. Both techniques involve the injection of bone cement into the vertebra to stabilize the fracture. Vertebroplasty “sets” the vertebra in its fractured position; balloon kyphoplasty uses orthopaedic balloons to return the vertebra to its original shape (when possible) before stabilizing the fracture with bone cement.